Myelofibrosis diagnosis
Diagnosing myelofibrosis, a rare blood cancer, usually involves a combination of physical exams, blood tests, imaging studies, and bone marrow tests.
Myelofibrosis is a myeloproliferative neoplasm (MPN), a blood cancer in which the bone marrow produces too many cells. Blood cell precursors acquire genetic mutations and begin overproducing immature or abnormal blood cells, which, in turn, cause inflammation and scarring (fibrosis) that further impair the bone marrow.
Reaching a myelofibrosis diagnosis can be difficult because it’s a rare condition that may overlap with other blood disorders. It also often develops slowly and might not cause obvious symptoms for a long time.
At the time of diagnosis, doctors will classify the disease by type and risk of progression, which informs the prognosis and optimal treatment strategy.
Signs and symptoms that lead to a diagnosis
Myelofibrosis might not cause symptoms for several years and is often detected incidentally during routine blood tests. But in other cases, the first evaluations occur when a person starts to notice symptoms such as:
- abdominal fullness and/or pain, or feeling full after eating very little
- extreme fatigue, weakness, or shortness of breath
- night sweats or unexplained fevers
- itching
- bone or joint pain
- unexplained weight loss
- easy bruising or bleeding
- frequent infections
Many of these symptoms can overlap with those of other blood disorders. If they arise, individuals should be referred to a hematologist or hematologist-oncologist, who can run more tests to identify their cause.
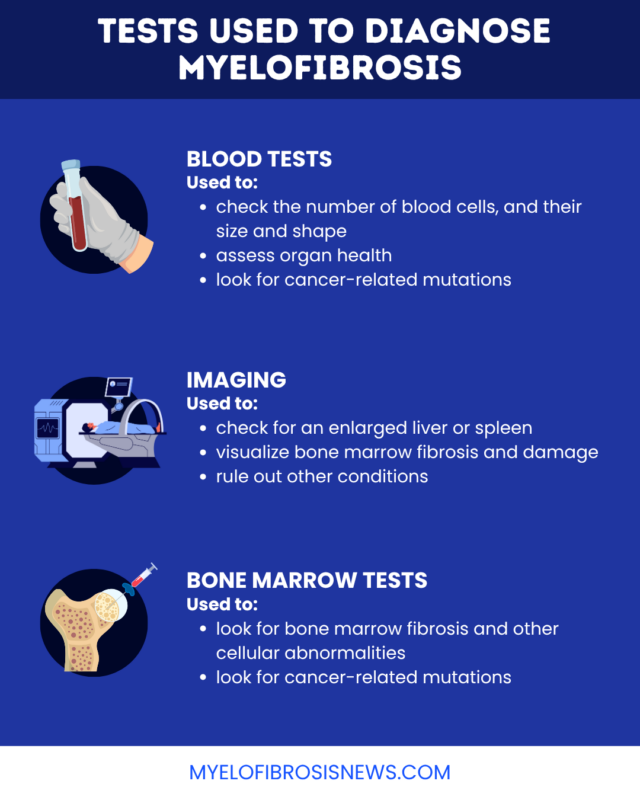
Diagnostic tests
Reaching a myelofibrosis diagnosis usually starts with a physical exam. A specialist will ask more about symptom history and feel the abdomen to check for signs of an enlarged spleen and liver. After that, they’ll likely run additional tests for myelofibrosis, including:
- blood tests
- imaging tests
- bone marrow aspiration and biopsy
Blood tests
A complete blood count test will look for changes in the numbers of blood cells, including red blood cells, white blood cells, and platelets. Blood cell counts are abnormal in myelofibrosis, and may be high or low depending on the disease stage and type.
Doctors may also examine blood cells under a microscope to see if they are abnormal in shape or size, in a so-called peripheral blood smear. Teardrop-shaped red blood cells are a possible sign of myelofibrosis.
Myelofibrosis blood tests may also look for other general markers of tissue injury and organ health.
Imaging tests
Imaging tests, including ultrasound and CT scans, can help doctors visualize the spleen and liver to see if they are larger than usual, which is common in myelofibrosis. An MRI scan can also show bone marrow fibrosis, another hallmark feature of the disease.
These tests may also help rule out other conditions that cause similar symptoms, such as lymphoma.
Bone marrow tests
Most people will need bone marrow tests to establish the diagnosis of myelofibrosis. With a bone marrow aspiration and biopsy, a needle is inserted into a large bone to collect a sample of liquid (aspiration) and solid tissue (biopsy). The samples are sent to the lab, where scientists will look for signs of scarring and other abnormalities consistent with myelofibrosis.
The cells collected from a blood test or bone marrow biopsy for myelofibrosis might also be used for genetic testing to look for potential disease-driving mutations. Myelofibrosis genetic testing can help doctors make a diagnosis and determine the right treatment plan.
Diagnostic criteria
As part of a myelofibrosis diagnosis, doctors will determine whether the disease is primary (occurring without another underlying condition) or secondary (occurring in the context of another disorder). According to the World Health Organization criteria, a primary myelofibrosis diagnosis requires:
- unusually high production of abnormal platelet precursor cells and increased bone marrow activity
- presence of genetic mutations or other evidence that cells are cancerous
- exclusion of other blood disorders, including other blood cancers
Also, at least one of the following must be present:
- unexplained anemia, or a lack of healthy red blood cells
- high white blood cell counts
- enlarged spleen
- elevated levels of lactate dehydrogenase (LDH), a marker of tissue damage
- immature blood cells in circulation
The disease will also be classified by stage as either early (prefibrotic) or advanced (overt fibrotic), with prefibrotic disease showing little or no bone marrow scarring and overt fibrotic disease showing moderate or severe fibrosis.
Secondary myelofibrosis most often develops from other MPNs, namely polycythemia vera or essential thrombocythemia. Diagnostic criteria generally require a prior diagnosis of a precursor condition, new or worsening bone marrow scarring, and at least two typical myelofibrosis features:
- anemia
- immature blood cells in circulation
- enlarged spleen
- night sweats, unexplained fever, or weight loss
- elevated LDH
Risk categories
At the time of diagnosis, a doctor will also categorize a person’s disease as low-, intermediate-, or high-risk based on the overall clinical picture. This helps determine a person’s long-term outlook and will aid doctors in selecting the appropriate treatment and myelofibrosis monitoring plan.
Classically, the International Prognostic Scoring System (IPSS) is used for myelofibrosis risk stratification at diagnosis, and the Dynamic Prognostic Scoring System (DIPSS) score is used for monitoring throughout treatment. These scoring systems consider several factors, including blood cell counts, symptoms, and age. Newer scoring systems that account for genetic mutations in cancer cells are also sometimes used.
People in lower-risk groups often have disease that can be controlled for a long time, and treatment may not be needed right away. Those in higher-risk groups are more likely to require treatment soon after being diagnosed.
After diagnosis
After their diagnosis, patients should work with their care team to establish a treatment and monitoring plan that makes sense given their individual risk status. Treatment, if necessary, could include medications, surgery, or a stem cell transplant.
Frequent follow-up and close monitoring starting at the time of diagnosis are critical for all people with myelofibrosis to ensure the best possible outcomes. If a person’s risk status changes at any point, the treatment plan may need to be adjusted accordingly.
Myelofibrosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
 Fact-checked by
Fact-checked by