Myelofibrosis treatment
Myelofibrosis treatment is largely focused on managing symptoms, lowering the risk of complications, and improving quality of life for people with this rare blood cancer. Ongoing research is aimed at developing new disease-modifying therapies for myelofibrosis that may slow disease progression and help extend survival.
Myelofibrosis belongs to a group of blood cancers called myeloproliferative neoplasms. In the disease, abnormal blood cells are produced in excess in the bone marrow, driving inflammation and scarring (fibrosis) that eventually interferes with the production of healthy blood cells. The spleen, which tries to compensate by making more blood cells, often becomes enlarged.
For most people, myelofibrosis is a chronic condition that develops slowly and is generally not curable, but symptoms can be managed with careful monitoring and standard treatments. An allogeneic stem cell transplant is the only potentially curative option, but this is an intensive procedure that’s generally reserved for a subset of patients with high-risk disease who are fit enough to undergo it.
Factors that influence myelofibrosis treatment choices
The specific myelofibrosis treatment regimen depends on several factors, including:
- blood cell counts
- number of immature blood cells
- symptoms and their severity
- genetic mutations in cancer cells
- age
- blood transfusion dependency
- general health and co-existing medical conditions
At diagnosis, a doctor will use a risk scoring system to determine a person’s prognosis based on these factors, categorizing them as low-, intermediate-, or high-risk.
Some people with lower-risk disease who don’t have symptoms might not need treatment right away. Instead, they may undergo active monitoring, also known as watch and wait, with regular check-ups to track disease progression. This close monitoring continues until there are signs the disease is progressing enough to require treatment.
For others with more advanced or high-risk disease, treatment may need to be started right away. The approach may involve medications, supportive therapies, or a stem cell transplant, depending on individual circumstances and symptoms.
Medications
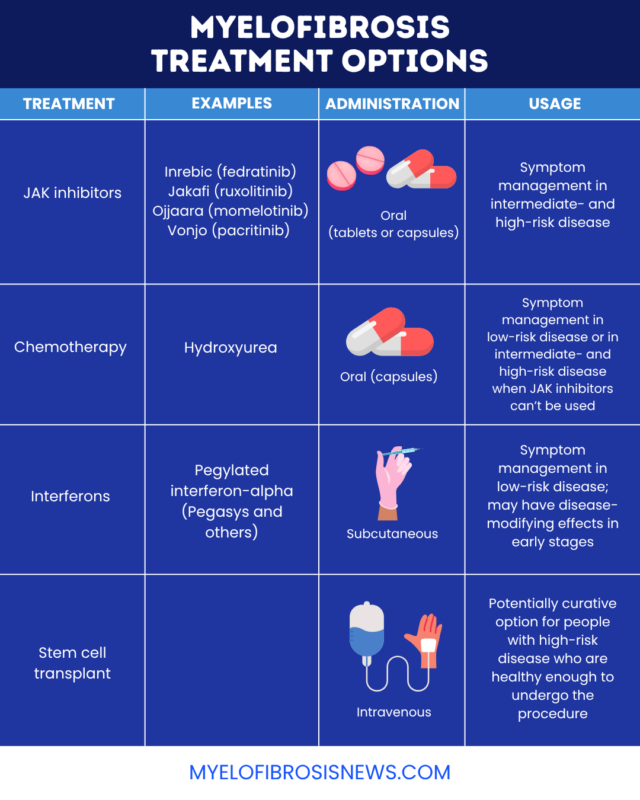
There are several myelofibrosis treatment options, selected based on disease stage, specific symptoms, and other factors.
JAK inhibitors
In most cases of myelofibrosis, cancer cells harbor mutations in one of three genes — JAK2, MPL, or CALR — which are associated with abnormal activation of the JAK/STAT signaling pathway. JAK inhibitor therapy is a standard first-line treatment option for managing intermediate- or high-risk myelofibrosis. There are four JAK inhibitors approved for myelofibrosis in the U.S.:
- Inrebic (fedratinib)
- Jakafi (ruxolitinib)
- Ojjaara (momelotinib)
- Vonjo (pacritinib)
All are taken orally as tablets or capsules. According to most treatment guidelines, Jakafi is a standard first-line choice. Vonjo may be preferred for people with severe thrombocytopenia, or low platelet counts, while Ojjara may be used for people with significant anemia, a lack of healthy red blood cells. Inrebic may be recommended for people who have failed or are intolerant to Jakafi.
JAK inhibitors are mainly used for spleen volume reduction (SVR) and to ease constitutional symptoms, such as fever, night sweats, and weight loss. They generally have limited effects on overall disease progression.
Chemotherapy
Chemotherapy, a class of cancer medications that work by killing fast-growing cells, is not a cornerstone of myelofibrosis treatment, but is sometimes used to ease symptoms associated with high blood cell counts in some people with low-risk myelofibrosis. The main chemotherapy agent used for this purpose in myelofibrosis is hydroxyurea, an oral medication.
Chemotherapy might also be used for intermediate or high-risk disease when JAK inhibitors don’t work well enough or cannot be tolerated.
Some people with myelofibrosis eventually develop acute myeloid leukemia (AML), a more aggressive blood cancer. These patients may receive other chemotherapy medications according to AML treatment guidelines.
Interferons
Pegylated interferon-alpha, sold in the U.S. as Pegasys and others, may be recommended for low-risk myelofibrosis, sometimes as an alternative to hydroxyurea or active monitoring.
Given via under-the-skin (subcutaneous) injections, the medication has immunomodulatory and anti-proliferative effects that help control the abnormal blood cell production seen in myelofibrosis. In early stages, pegylated interferon-alpha has been shown in some patients to slow bone marrow fibrosis and reduce the number of malignant cells, potentially exerting a disease-modifying effect.
Interferons may also be used in cases where JAK inhibitors are not safe, such as during pregnancy.
Stem cell transplant
An allogeneic stem cell transplant, sometimes called a bone marrow transplant for myelofibrosis, may be considered for a small number of people. Essentially, the procedure provides the body with blood stem cells from a donor to help repopulate the bone marrow with healthy blood cells. The process involves:
- A course of high-dose chemotherapy to eliminate abnormal bone marrow cells
- Infusion of stem cells collected from a healthy donor into the bloodstream
- Engraftment of the new stem cells in the bone marrow, where they start producing new healthy blood cells
Stem cell transplantation can extend survival and is currently the only potentially curative treatment for myelofibrosis. However, it is a very intensive treatment that has several risks and a long recovery time. As such, it is usually reserved for people with high-risk disease who are fit enough to undergo the procedure.
Supportive therapies
Treatment also relies heavily on supportive therapies for managing myelofibrosis symptoms and preventing complications. The specific therapies will vary on a case-by-case basis.
Anemia
One of the major goals of treatment is to manage anemia in myelofibrosis. Various medications may be used to help stimulate the bone marrow to make more red blood cells, including:
- erythropoietin, an injectable growth factor medication
- danazol, an oral steroid medication
- folic acid (vitamin B9) supplements
When anemia is severe, patients may receive blood transfusions to provide them with red blood cells from a healthy donor.
Spleen enlargement
An enlarged spleen, or splenomegaly, can be uncomfortable or painful. If medications don’t help, patients may undergo radiation therapy to help facilitate splenomegaly reduction. Radiation might also be used in cases where other organs, such as the liver, become enlarged and painful.
In some cases, a doctor may recommend surgery to remove the spleen, called a splenectomy. While a person can live without a spleen, the procedure carries risks, so it is not commonly performed.
Other symptoms
Other supportive therapies for myelofibrosis could include:
- aspirin, to prevent blood clots
- allopurinol, an oral medication to manage gout, a painful form of inflammatory arthritis
People with myelofibrosis may have a weakened immune system. They may be given antibiotic or antiviral medications to prevent serious infections, and are advised to get all recommended vaccinations to help manage infection risk.
Lifestyle and symptom management
As with most chronic conditions, people with myelofibrosis can make lifestyle adjustments that help make it easier to live with the blood cancer, including:
- eating a balanced diet that meets all nutritional needs and staying hydrated
- quitting smoking
- engaging in regular exercise, as tolerated and tailored to individual abilities
- getting enough rest
- participating in counseling or support groups for mental health
While these changes can’t cure myelofibrosis, they can help improve quality of life and make daily activities easier.
It is also very important that people with myelofibrosis follow a regular monitoring and follow-up plan with their care team. This allows doctors to promptly identify changes in their condition and make treatment adjustments as needed.
Myelofibrosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
 Fact-checked by
Fact-checked by