Myelofibrosis overview
Myelofibrosis is a rare condition belonging to a group of blood cancers called myeloproliferative neoplasms (MPNs).
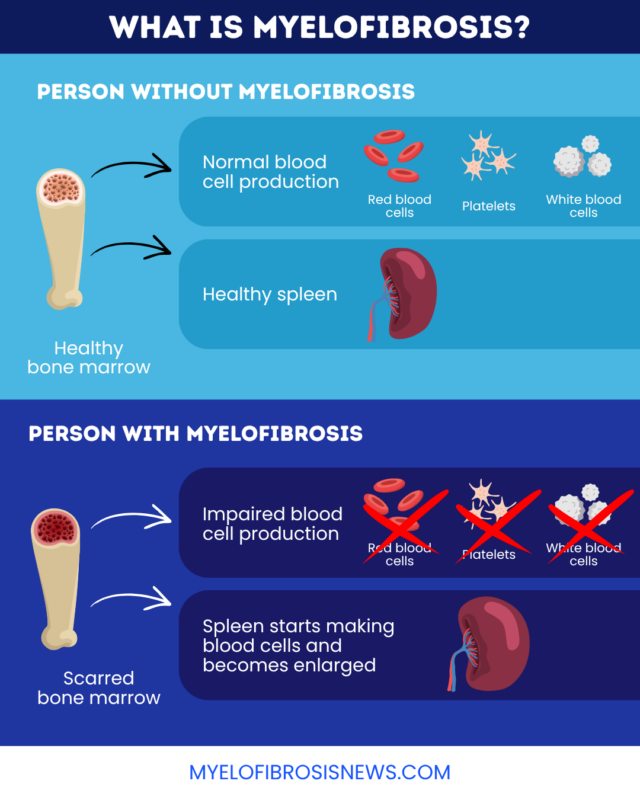
In its early stages, large amounts of abnormal blood cells are produced in the spongy center of bones, known as the bone marrow. Over time, these cancerous cells cause inflammation and scarring (fibrosis) in the marrow that inhibit the production of healthy blood cells, leading to blood cell deficiencies and related symptoms. The spleen, which tries to compensate by producing blood cells, becomes enlarged.
The course of myelofibrosis can vary widely. For many, it is a slow-growing, chronic cancer that takes years to cause significant symptoms. For others, the disease progresses quickly and could transform into a more aggressive type of leukemia.
Most people with myelofibrosis won’t be cured, but there are treatments to help ease symptoms, prevent complications, and improve overall life quality.
Causes and risk factors
Scientists don’t know exactly why myelofibrosis happens. It usually develops in people without known blood or bone marrow problems, but may sometimes arise in people with existing blood conditions.
The disease is thought to occur when hematopoietic stem cells, the precursors to mature blood cells, spontaneously acquire mutations that cause them to grow and divide uncontrollably, producing large amounts of abnormal blood cells. For most people, myelofibrosis is associated with mutations in one of three genes: JAK2, CALR, or MPL.
Ultimately, those abnormal cells release inflammatory molecules that cause the disease’s characteristic bone marrow scarring.
While anyone can develop myelofibrosis, risk factors for the disease include:
- older age
- preexisting blood disorders
- exposure to benzene or other industrial chemicals
- exposure to high levels of radiation
Types
Myelofibrosis is categorized into two main types based on its origin:
- Primary myelofibrosis develops spontaneously without a precursor condition.
- Secondary myelofibrosis develops when other disorders, usually the MPNs essential thrombocythemia or polycythemia vera, progress to cause bone marrow scarring.
These two disease types generally have similar symptoms and treatment options. At diagnosis, doctors will also classify myelofibrosis into a risk category that informs a person’s long-term prognosis and treatment choices, regardless of whether the disease is primary or secondary.
Various risk stratification tools may be used, which take into account symptoms, blood cell counts, genetics, age, and other factors to determine the likelihood of disease progression.
Symptoms
Myelofibrosis does not always cause obvious symptoms, especially in earlier stages before there is substantial bone marrow fibrosis. When symptoms do occur, they may include:
- fatigue or weakness
- shortness of breath
- easy bruising or bleeding
- frequent infections
- night sweats and fevers
- itchy skin
- bone or joint pain
- unexplained weight loss
- problems with concentration
- abdominal pain or fullness
- feeling full after eating only a little food
- nausea or digestive issues
These common symptoms are mainly related to low blood cell counts (cytopenias), spleen enlargement (splenomegaly), and systemic inflammation.
Other possible symptoms and complications include:
- gouty arthritis, a painful inflammatory joint condition
- blood cell production outside the bone marrow
- serious blood clotting complications, such as a heart attack or stroke
- severe bleeding
Around 10%-20% of people with myelofibrosis will progress to develop acute myeloid leukemia (AML), a more aggressive type of blood cancer.
Diagnosis
Reaching a myelofibrosis diagnosis usually involves:
- a physical exam and thorough medical history review, to look for signs of myelofibrosis, such as an enlarged spleen
- blood tests, to look for abnormalities in blood cell counts, size, or shape
- imaging tests, to detect spleen and liver enlargement or bone marrow changes
- bone marrow biopsy and aspiration, to identify cancerous cells and fibrosis
Blood and bone marrow samples may also be used for genetic testing to identify which, if any, mutations might be associated with the cancer.
Doctors use the results of these tests to determine whether the diagnostic criteria for primary or secondary myelofibrosis are met. They’ll also use that information to determine a person’s risk group.
Treatment
Myelofibrosis treatment focuses largely on controlling symptoms, preventing complications, and improving quality of life.
The specific treatment choice depends on several factors, including symptoms, age, general health, and genetics. Some people with early or low-risk disease don’t need to be treated right away, but will instead be closely monitored for disease progression.
For those who do need treatment, it may include:
- JAK inhibitors: Used largely for managing spleen enlargement or other symptoms in people with intermediate- or high-risk disease. Include Inrebic (fedratinib), Jakafi (ruxolitinib), Ojjaara (momelotinib), and Vonjo (pacritinib).
- Chemotherapy: Used to manage high blood cell counts.
- Interferons: May be used for symptom management in people with low-risk disease.
For the most part, these medications can help shrink the spleen and relieve constitutional symptoms such as fatigue, but most do not substantially slow disease progression.
Supportive care is also key and may include medications or blood transfusions for red blood cell deficiencies (anemia), and less commonly, surgery or radiation therapy for severe spleen enlargement.
An allogeneic stem cell transplant is the only potential cure for myelofibrosis. It uses high-dose chemotherapy to wipe out diseased bone marrow cells, followed by an infusion of healthy donor stem cells to repopulate the marrow with healthy blood cells. This is a very intensive procedure that comes with several risks, and is generally reserved for a small number of patients with high-risk disease who are young and healthy enough to undergo it.
Disease progression and prognosis
The course of myelofibrosis can be variable, but for many, it gradually progresses over years. The exact course of the disease depends on many factors, including:
- age
- blood cell counts
- symptoms
- genetic mutations
- general health and coexisting conditions
- disease type and subtype
A person’s risk score at diagnosis and throughout treatment, which is influenced by all of these factors, informs the likelihood of disease progression and survival.
Reported overall survival rates for people with myelofibrosis vary widely, ranging from fewer than two years to over 15 years post-diagnosis, depending on risk scores. About 10%-20% of people progress to develop AML, which substantially affects survival.
Most current treatments have a limited ability to slow disease progression and extend survival, but modern treatments may help patients live longer. Some JAK inhibitors have a modest effect on survival, and a stem cell transplant in eligible high-risk patients can be curative.
Living with myelofibrosis
For most, myelofibrosis is a chronic condition that can have a substantial impact on daily life. There are a few steps patients can take to make coping with the rare blood cancer easier, including:
- eating a healthy diet and staying hydrated
- staying active
- getting enough rest and conserving energy to manage fatigue
- getting all recommended vaccines and practicing good hygiene to avoid infections
- adhering to a regular monitoring and follow-up schedule
Myelofibrosis can take an emotional toll on both patients and caregivers. Mental health support, such as counseling or support groups, is also a key aspect of living well with myelofibrosis.
Myelofibrosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
 Fact-checked by
Fact-checked by